Abstract
Summary: Perfluoro-n-octane (PFO) is a heavy liquid that is used as an aid for complicated retinal surgical procedures. Although PFO is usually removed intraoperatively, the radiographic appearance of retained PFO may mimic an intraocular foreign body or vitreous hemorrhage. As the use of PFO in retinal procedures has become more widespread, recognition of its imaging appearance has become important in the differential diagnosis of intraocular foreign body and ocular trauma.
Perfluoro-n-octane (PFO) is a perfluorocarbon liquid (PFCL) that has been used as an aid for the surgical repair of complicated proliferative vitreoretinopathy and giant retinal tears since 1987 (1). Its high density and low viscosity allow PFO to provide a significant tamponade force that stabilizes the retina and gives the surgeon the ability to manipulate the retina with greater ease. These properties have brought PFO into widespread use by retina surgeons for these types of procedures. PFO is removed intraoperatively because of the risk of ocular toxicity if it is left in the vitreous cavity (2). A small amount of PFO may be inadvertently left in the vitreous cavity postoperatively, however, and retained PFCL in the vitreous cavity after surgery has been reported in 1–38% of cases (3, 4). Because of its high density, PFO may appear radiopaque and thus may mimic an intraocular foreign body or hemorrhagic collection. As the use of PFO in retinal surgery becomes more widespread, its recognition on orbital images has become important.
Case Report
A 50-year-old woman was referred to our clinic for evaluation of an intraocular foreign body. The patient had been in a motor vehicle accident several days earlier and had complained of headaches.
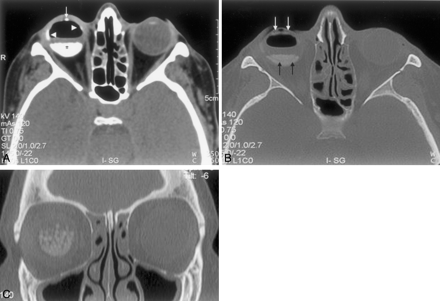
A nonenhanced multidetector CT scan was performed in the axial plane with coronal and sagittal reformats in bone and soft tissue algorithms. The CT scan showed an dense fluid collection (H 454–585) representing PFO layering dependently within the posterior globe (Fig 1A). There were two principal components, one layering within the posterior vitreous chamber and forming a fluid-fluid level with the native vitreous humor and the second extending along the subretinal space to the level of the ora serrata. There was an abnormal linear attenuation floating between these two components, representing the detached retina (Fig 1B). Several punctate densities corresponding to additional foci of PFO were noted within the vitreous cavity (Fig 1C). There was no evidence of fracture or dislocation and no evidence of other intra- or periorbital foreign body.
A, Axial CT scan without contrast demonstrates attenuated fluid collection within the posterior vitreous cavity (asterisk) and smaller deposits in the ora serrata region (arrowheads) forming a fluid-fluid level with the native vitreous humor. PFO can also be seen within the anterior chamber (white arrow).
B, Axial CT with bone algorithm and bone windows demonstrates a retinal detachment (black arrows) and the two components of the collection, the one anterior to the detached retina and the second within the subretinal space extending to the ora serrata. PFO is also seen within the anterior chamber (white arrows).
C, Coronal CT reformat with bone windows demonstrates the corrugated surface of the PFO collection corresponding to the PFO bubbles seen intraoperatively.
The patient’s ocular history was remarkable for recurrent retinal detachment with proliferative vitreoretinopathy in her right eye. She had undergone four previous surgical repair attempts. PFO had been used during the last surgery, 5 weeks earlier; however, hemorrhage occurred intraoperatively, and the PFO could not be removed before closure.
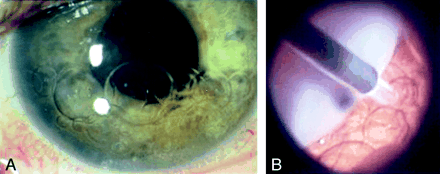
On her initial visit to our clinic, the patient’s visual acuity in the right eye was hand motion at 6 inches. The anterior segment examination revealed multiple PFO bubbles (Fig 2A), and the fundus examination showed PFO overlaying a detached retina. There were no corneal or scleral lacerations, and the rest of her physical examination was unremarkable. Subsequently, the patient was taken to surgery, where the PFO was seen in the preretinal and subretinal spaces without significant hemorrhage (Figs 2B). The PFO was removed and the retina reattached surgically.
A, External view of the eye showing multiple PFO bubbles over the inferior third of the anterior chamber.
B, Intraoperative view in the vitreous cavity showing the retracted opacified retina (upper left) and the extrusion canula removing multiple PFO bubbles from the subretinal space.
Phantom Study
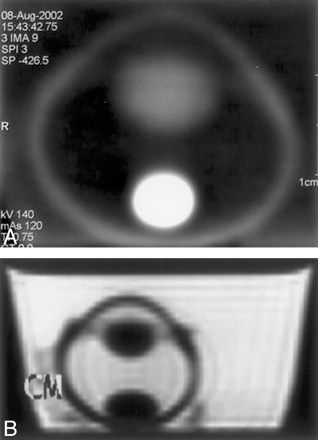
An enucleated porcine eye was injected with 0.5 mL of PFO (Perfluoron; Alcon Laboratories, Ft. Worth, TX). This was placed in an 8-ounce (237-mL) polystyrene container filled with water, which has similar radiodensity as vitreous humor, with the cornea turned superiorly. Nonenhanced CT and MR imaging were performed on the enucleated specimen in the axial plane. CT showed the PFO as an attenuated, round, smoothly marginated globular fluid collection (H 643–673) in the dependent portion of the posterior vitreous cavity (Fig 3A). T1- and T2-weighted MR imaging showed the PFO as an oval hypointense collection layering dependently without significant chemical shift artifact (Fig 3B).
A, Axial nonenhanced CT image of an enucleated porcine globe demonstrates the attenuated smoothly marginated globule of PFO deposited into the vitreous cavity.
B, T2-weighted MR image of an enucleated porcine globe demonstrates a hypointense oval collection lying dependently in the vitreous cavity.
Discussion
PFO (C8F18) is a colorless, odorless synthetic fully fluorinated carbon compound. It possesses a high density (1.76 specific gravity) and low viscosity (0.8 centistokes) (5). These properties make PFO a highly desirable substance for retinal surgery because it provides a significant tamponade force that helps to stabilize the retina intraoperatively. This allows other maneuvers to be done on the retina, such as extrusion of subretinal fluid, manipulation of retinal edges, or the application of laser treatment. As a result, the use of PFO for complex retinal surgical procedures has become more widespread. PFO is removed from the vitreous cavity after its intraoperative use because of the potential for ocular toxicity, including retinal inflammation and atrophy of the dependent retina from mechanical compression (2).
CT shows PFO as an attenuated fluid that may layer within the compartment where it is placed, usually anterior to the retina within the vitreous chamber. It may extrude into the subretinal space through an opening in the retina, as was seen in this case. PFO may mimic a dense hemorrhage or a metallic or dense foreign body. The Houndsfield attenuation in this case may be helpful in distinguishing the PFO collection from vitreous or subretinal hemorrhage, because PFO demonstrates a higher attenuation value than that of blood products as in our case, H 454–585 in the human subject and H 643–673 in the enucleated porcine specimen.
The volume of residual PFO seen postoperatively is usually less than that seen in our case. It is often one or more droplets, which may resemble small intraocular foreign bodies on CT scans. In the experimental porcine eye, PFO formed a rounded globule with smooth margins within the posterior vitreous and, in such cases, may mimic a focal foreign body such as a BB. Correlation with a clinical history of previous retinal surgery is important in forming the differential diagnosis. Imaging findings that may aid in the diagnosis of intraocular PFO include the high Houndsfield attenuation on CT or hypointensity on MR imaging, the corrugated surface appearance of the collection corresponding to the PFO bubbles, and lack of streak artifact on CT, which may occur with metallic foreign bodies but is not seen with PFO.
Conclusion
PFO is a heavy liquid that is used as an aid for complicated retinal surgical procedures. A small amount of PFO is often left behind in the vitreous cavity postoperatively. Because of its high Hounsfield attenuation and radiopaque properties, PFO should be part of the differential diagnosis of intraocular opacities when seen on CT scan.
Footnotes
Supported in part by the Vitreoretinal Research Fund (to D.J.D’A.) and the Iacocca Research Foundation.
- Received November 11, 2002.
- Accepted after revision April 6, 2003.
- Copyright © American Society of Neuroradiology