Abstract
BACKGROUND AND PURPOSE: Cervicofacial actinomycosis is uncommon, but without proper treatment it causes extensive tissue destruction. Early diagnosis is critical but usually difficult with cultures or imaging. Our aim was to identify characteristic imaging features that facilitated diagnosis in seven patients with cervicofacial actinomycosis.
METHODS: We retrospectively reviewed the CT and MR findings in seven patients with pathologically proved actinomycosis. Histologic diagnosis was made by means of surgical excision or biopsy in seven patients. Culturing was performed in two patients. Enhanced CT scans (n=7) and MR images (n=2) were evaluated for the location, margin, infiltrative nature, enhancement pattern, and presence of lymphadenopathy.
RESULTS: CT and MR images showed either a well-defined (n=2) or ill-defined (n=5) mass. Involved areas included the nasal cavity (n=2), buccal space (n=1), pyriform sinus (n=1), aryepiglottic fold (n=1), oro- and hypopharynx (n=1) and tongue (n=1). Imaging confirmed the infiltrative nature, showing the tendency of the lesion to invade across tissue planes and boundaries (n=6). Moderate homogeneous contrast enhancement was seen on CT scans in six patients with several small low-attenuating foci (n=2). T1- and T2-weighted MR images showed intermediate signal intensity with moderate contrast enhancement (n=2). Reactive lymphadenopathy was associated in three patients.
CONCLUSION: Although cervicofacial actinomycosis occurs infrequently, it should be included in the differential diagnosis when images show a soft-tissue mass with inflammatory changes and an infiltrative nature in the cervicofacial area.
Actinomycosis is an uncommon disease caused by Actinomyces species, gram-positive anaerobic bacteria and normal inhabitants in the oral cavity and respiratory and digestive tracts. Actinomyces israelii is the most common pathogen resulting in actinomycotic infection. Clinical manifestation occurs in one of three forms: cervicofacial, abdominal-pelvic, or pulmonary actinomycosis. Cervicofacial actinomycosis accounts for about 50% of the cases. Diagnosis may be difficult because of a general lack of familiarity with the disease and a low success rate in culturing the organism as a result of its fastidious nature (1). Early diagnosis is critical to initiate proper antibiotic therapy and to prevent extensive local tissue destruction.
Few reports describe the imaging findings of cervicofacial actinomycosis (2, 3); all of these characterized the findings as nonspecific. Over 9 years, we collected seven cases of cervicofacial actinomycosis and reviewed the CT and MR findings to determine the imaging features suggestive of cervicofacial actinomycosis.
Methods
Between 1992 and 2000, we reviewed the records of seven patients with pathologically proved cervicofacial actinomycosis. These patients included two male and five female patients aged 6–80 years (6, 24, 41, 49, 61, 77, 80 years; mean, 48 years). Both the duration of symptoms and the chief presenting complaint were evaluated. The preoperative initial imaging diagnosis was reviewed. The histologic diagnosis was established after surgical excision in five patients and after biopsy in two patients (case 4, case 6). Preoperative microbiologic cultures were obtained in two patients (case 1, case 2) by aspirating a mass before surgery. The results revealed actinomycosis in one patient. Contrast-enhanced CT was performed in all patients (precontrast scans were obtained in two patients), and MR imaging was performed in two patients before surgery.
Two radiologists retrospectively reviewed the CT and MR images. The location, margin, infiltrative nature of the lesion, degree and homogeneity of the contrast enhancement, and the lymph nodes were categorized by consensus. The margins of the lesions were classified as well or ill defined. A well-defined lesion was defined as a lesion without any notable infiltration of the adjacent fat or soft-tissue planes. An infiltrative lesion was defined as the presence of invasion or crossing the adjacent soft-tissue planes. The degree of contrast enhancement was classified as mild (similar to muscle enhancement) or moderate (prominent and more enhancement than in muscle but less than that in the carotid artery).
Results
The duration of symptoms before diagnosis ranged from 2 weeks to 5 months (average, 6 weeks). A palpable, tender mass was present in three patients. Other symptoms included hoarseness, nasal obstruction, headache, tongue pain, and fever. A precipitating event was noted in one patient; this was previous maxillary sinus surgery to treat sinusitis. The locations of the lesions included the nasal cavity (n=2), gingival and buccal space (n=1), hypopharynx (n=1), medial aspect of aryepiglottic fold (n=1), oropharynx and hypopharynx (n=1), and tongue (n=1).
The imaging features are summarized in the Table 1. Before histologic confirmation, the suggested radiologic diagnosis was malignancy (n=4; cases 2, 4, 5, and 6) or fungal infection (n=1; case 7). In two cases, the differential diagnosis was between malignancy and a granulomatous lesion, such as tuberculosis (case 1) or an infectious process (case 3); the differentiation was difficult. The suggested clinical diagnosis was a neoplasm (n=4; cases 1, 4, 5, and 6), tuberculous infection (n=1; case 3), or fungal infection (n=1; case 7). A buccal-space mass was thought to be a postoperative mucocele on the basis of the clinical findings (case 2).
Imaging features of cervicofacial actinomycosis
On imaging studies, the lesions had ill-defined margins due to surrounding inflammatory response in five cases (Fig 1A) or well-defined margins in two cases (Fig 2). Imaging results confirmed the infiltrative nature of the lesion, which had a tendency to extend into the adjacent neck space; it crossed more than one tissue plane and boundary in six patients (Fig 3). In one case, the lesion was limited to the aryepiglottic fold (Fig 4). All cases presented with soft-tissue masses without substantial necrosis; no cystic lesions were found on imaging studies. Nonenhanced CT scans showed soft-tissue masses with isoattenuation relative to muscle in two cases. In one case in our study, popcorn-like dystrophic calcification within the mass was found in a lesion in the nasal cavity. Of the seven cases, images in six cases showed moderate contrast enhancement (Figs 3 and 4). Only one case showed mild contrast enhancement. All cases showed relatively homogeneous contrast enhancement. Two of our study cases showed a small, hypoattenuated area in the central portion of the mass (Figs 1 and 3C). Pathologically, this hypoattenuated area was confirmed to be composed of actinomycotic granules with a small adjacent necrotic portion surrounded by granulation tissue and fibrosis (Fig 1B).
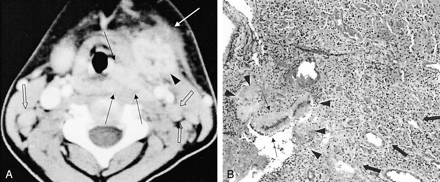
Case 1. A 6-year-old girl with an ill-defined lesion of the left pyriform sinus.
A, Contrast-enhanced axial CT scan shows a moderately enhancing mass (black arrows) in the left pyriform sinus. It extends to the submandibular gland (arrowhead) and platysma muscle (white arrow). The left submandibular gland is enlarged and has multiple small nonenhancing portions. Multiple, small, homogeneous, well-defined oval lymph nodes are found in both internal jugular chains (open arrows).
B, Photomicrograph of a specimen shows actinomycotic granules (thin arrows) and adjacent necrosis (arrowheads). These are surrounded by granulation tissue and fibrosis (thick arrows) (hematoxylin-eosin stain, original magnification ×200).
Case 2. A 77-year-old woman with a well-defined buccal-space lesion.
A, Contrast-enhanced axial CT scan shows an elliptical mass (arrows), which extends from the gingiva to the right buccal space. This mass shows moderate contrast enhancement without fat infiltration.
B, Same CT scan obtained with a bone setting shows the mass (arrows).
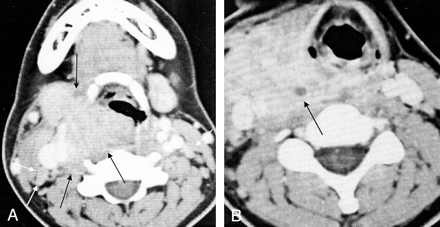
Case 3. A 24-year-old woman with an oro- and hypopharyngeal lesion.
A, Contrast-enhanced axial CT scan shows a soft-tissue mass in the right hypopharynx (black arrows). The mass extends to the submandibular gland and to the retropharyngeal, prevertebral, and carotid spaces. This lesion shows moderate contrast enhancement. Several lymph nodes are found in the both internal jugular chains (white arrows).
B, Contrast-enhanced axial CT scan shows a bulky mass with moderate contrast enhancement in the right visceral space. The mass extends to the retropharyngeal space, carotid space, and sternocleidomastoid muscle. A small nonenhancing portion, suggestive of necrotic foci, is found in the mass (arrow).
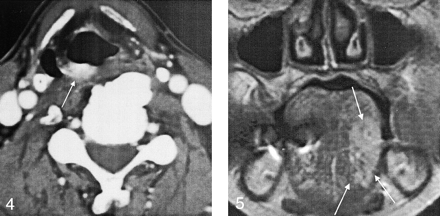
Case 4. A 61-year-old man with a lesion of the aryepiglottic fold. Contrast-enhanced axial CT scan shows a moderately enhancing soft-tissue lesion in the right aryepiglottic fold (arrow). This lesion has a relatively well-defined margin and no notable extension into the adjacent soft tissue.
Cervical lymph nodes could be evaluated in four cases. Borderline lymph node enlargement (not larger than 1 cm in diameter) was seen in three patients. These lymph nodes showed mild to moderate enhancement and well-defined margins (Figs 1A and 3A).
In two cases studied with MR imaging, T1- and T2-weighted images showed a similar infiltrative mass that was isointense relative to muscle (n=2) (Figs 5 and 6). In one case, involvement of the cavernous sinus with narrowing of the internal carotid artery was present (Fig 6). Contrast-enhanced T1-weighted images showed strong contrast enhancement (Figs 5 and 6C).
Case 5. A 80-year-old woman with a tongue lesion. Coronal contrast-enhanced fat-saturated T1-weighted MR image (TR/TE, 533/16) shows a mass with moderate contrast enhancement (arrow).
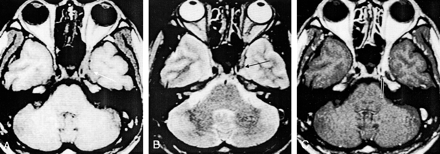
Case 6. A 41-year-old man with a nasal-cavity lesion.
A, Axial T1-weighted MR image (480/20) shows an elongated lesion with intermediate signal intensity in the left cavernous sinus and orbital apex (arrow).
B, Axial T2-weighted MR image (2630/80) shows a mass of intermediate signal intensity (arrow).
C, Contrast-enhanced T1-weighted MR image (480/20) shows diffuse contrast enhancement and narrowing of the internal carotid artery (arrow).
All patients were treated by means of mass excision and were given high doses of penicillin or ampicillin. A recurrent lesion developed in only one case; this was successfully treated with abscess aspiration and high doses of penicillin.
Discussion
The most common physical finding of actinomycosis is a woody, hard, palpable mass with a subacute clinical course. About half of the patients present with a low-grade fever (1). The lack of responsiveness to empirical antibiotic therapy, the presentation of a chronic palpable mass, and the difficulty in establishing the microbiologic diagnosis make it difficult to differentiate this mass from a neoplasm, granulomatous disease, or a fungal infection on the basis of the initial presentation (1, 4).
Actinomyces species are anaerobic bacteria that cannot penetrate healthy tissue, and mucosal breakdown is a prerequisite for infection. About half of the patients have a history of local trauma resulting in mucosal breakdown (1). Poor dental hygiene, caries, oral trauma, dental extraction, and an immunocompromised status are considered to be important antecedents (1, 4). Determining if a patient has a history of these risk factors may be helpful in establishing a correct diagnosis. In cervicofacial actinomycosis, commonly involved sites include the submandibular space, cheek, parotid gland, teeth, and tongue, among others (1, 4, 5–7).
Actinomycosis is diagnosed by examining the exudate and infected tissue. Gram staining reveals gram-positive long-branching filaments. The histologic and microscopic diagnoses are made by the finding of sulfur granules in the specimens. Microbiologic identification is often difficult because this organism grows slowly, and careful anaerobic culturing is required. Therefore, incisional biopsy is often undertaken to determine a diagnosis (1, 5, 7).
Few reports describe the imaging findings of cervicofacial actinomycosis. CT findings of cervicofacial actinomycosis include an enhancing soft-tissue mass with a low-attenuating center associated with inflammatory change in the adjacent soft tissue (2, 3, 8). Invasion of the adjacent soft tissue, including the muscles, can occur. In our study, most lesions appeared as ill-defined, infiltrative, soft-tissue masses with an inflammatory reaction. The lesions of the nasal, oral, and pharyngeal cavities contiguously extended to the adjacent neck space, crossing fascial planes. This infiltrative nature is also reported in the abdominopelvic and thoracic actinomycosis (9, 10), and it may be attributed to the actions of the proteolytic enzymes of the organism (9). Not all actinomycoses result in an infiltrative mass, and in two cases in out study, the lesion appeared as a localized mass. The radiologic finding may be affected by the course of the disease, any previous antibiotic therapy, and the immune status of the host. In the subacute stage, actinomycosis may result in a slowly progressing, infiltrative mass if not properly treated, as in our cases. If imaging is performed in the acute phase, actinomycosis may be seen as a localized mass.
Another imaging feature was the moderate, relatively homogeneous contrast enhancement of the lesion. No large necrotic areas or cystic portions were observed in the actinomycosis mass. Two cases in our study showed small, central areas of low attenuation, similar to the findings in previous reports. This enhancement pattern may be related to the histologic nature of actinomycosis, which includes a central suppurative necrosis surrounded by granulation tissue and intense fibrosis (11). Abundant granulation and attenuating fibrous tissues in the mass may cause marked contrast enhancement. Central suppurative necrosis may appear as a nonenhancing portion in the mass.
The organism causing actinomycosis usually does not spread via the lymphatic system because of the size of the bacterium; regional lymphadenopathy is uncommon or it develops late (1, 12). However, regional lymphadenopathy was noted in as many as 40% of the cases in some studies (1, 3). In our study, mild reactive lymphadenopathy was found in only three cases.
T1- and T2-weighted MR images showed an intermediate signal intensity associated with moderate contrast enhancement. This signal intensity characteristic may be associated with the histologic feature of abundant granulation and fibrous tissue in actinomycosis.
Popcorn-like dystrophic calcification was found in one case of our study. To our knowledge, no previous reports have described calcification in actinomycosis. In our study, this calcification may have been caused by chronic inflammation, which causes tissue necrosis and eventual dystrophic calcification (13).
Cervicofacial actinomycosis may mimic either a malignant neoplasm of the head and neck or a chronic granulomatous lesion, such as that due to tuberculosis or a fungal infection (4). A malignant neoplasm may also result in an enhancing solid mass, but the lesion usually has a relatively well-defined margin, without substantial inflammatory change in the adjacent soft-tissue unless it is complicated by infection. The lack of lymphadenopathy despite a large, aggressive-appearing mass with an inflammatory change may be a helpful clue in differentiating cervicofacial actinomycosis from a malignancy.
Cervical infection due to tuberculosis or a fungal infection, such as coccidioidomycosis, usually presents with matted cervical lymphadenopathy (8). The nodal distribution of these diseases and the lymph node characteristics may be helpful in differentiating cervicofacial actinomycosis from these diseases. Ultimately, culture and histologic analysis are required.
Conclusion
Actinomycosis should be included in the differential diagnosis of a relatively homogeneously enhancing soft-tissue mass associated with substantial inflammatory reaction and infiltration of the cervicofacial area. The area of necrosis in the mass of actinomycosis is small, if present. Actinomycosis is accompanied by a few reactive cervical lymph nodes, despite the large size of the mass.
References
- Received February 5, 2002.
- Accepted after revision September 12, 2002.
- Copyright © American Society of Neuroradiology